We are here to support you.
Click here to get in touch and book online: Contact us

Support
Whether you’re accessing abortion, vasectomy or contraception care with MSI UK, we are here to support you throughout your journey.
Who we are
We’re the leading provider of sexual and reproductive health services in the UK.
Find a clinic
We have over 60 clinics across Englan. Select a location to see the list of clinics available.
Blog
Read news, personal stories from our clients, and find out how you can help millions of people around the world access safe abortion.
Abortion • 7 June 2022 • 4 min read
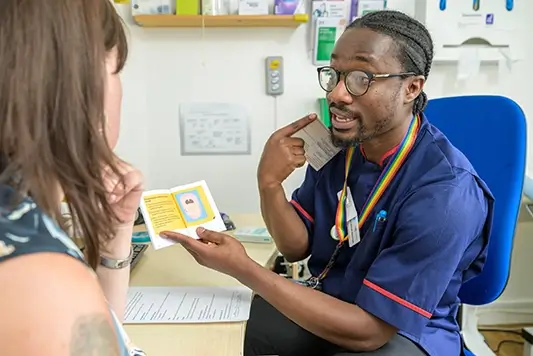
A client shares her medical abortion story
“At the time of my abortion, I read every client’s story on this website, and I told myself I would have to write my own.”
Latest posts


Abortion
Advocacy
Contraception
News from MSI UK
Press releases
Stories
Vasectomy
Abortion
Abortion
Contraception
Contraception
Decriminalisation of abortion care
In the news
Information and advice
Information and advice
Information and advice
Interviews with MSI UK staff
Law
Law changes
Medical abortion
Myth busting
Myth-busting
Recovery and aftercare
Recovery and aftercare
Reproductive rights
Safe access zones
Services
Stories
Stories
Surgical abortion
Latest posts


Stories

19 April 2024 • 2 min read
I wasn’t ready to be a parent at 20 – my abortion story
“About 20 minutes after I realised my pregnancy test was positive, I was on the phone to MSI UK.”
Stories

19 April 2024 • 6 min read
Abortion story: I believe my at-home abortion saved my life
“The attention, care and rapid response I received, I believe saved my life.”
News
12 April 2024 • 9 min read
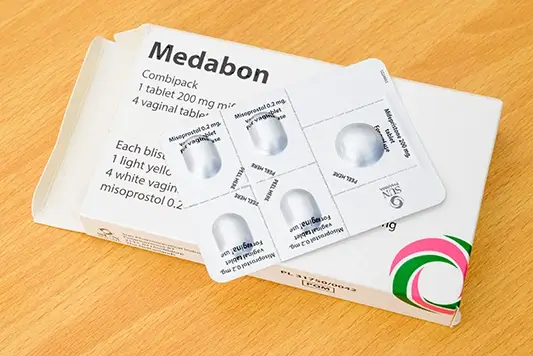
The abortion pill process
Read our blog to learn about the abortion pill process and how a medical abortion works.
Stories

26 March 2024 • 4 min read
My story: Choosing an abortion as someone who’s already a mum
“Prioritising our family felt like the right decision.”
News

13 March 2024 • 7 min read
Why would anyone have an abortion outside the law?
Learn what may lead to people having an abortion outside the law, and why we believe no one should face prosecution.
News

21 February 2024 • 2 min read
New paper calls for abortion law reform across the UK
A paper published in the International Journal of Gynaecology and Obstetrics (IJOG) calls for UK abortion law reform.
News

19 February 2024 • 8 min read
Why we back Diana Johnson’s amendment to the Criminal Justice Bill
Abortion is healthcare, not a crime. Learn why we back Diana Johnson’s amendment to the Criminal Justice Bill.
News

16 February 2024 • 3 min read
MSI’s transformative surgical abortion training featured in The Lancet
The Lancet has showcased the surgical abortion training offered by MSI UK’s Dr Yvonne Neubauer.
News

12 February 2024 • 3 min read
Ealing council renews Safe Access Zone around MSI UK’s West London clinic
Ealing Council has announced the decision to renew the Safe Access Zone protecting MSI UK’s West London clinic.


